Oral STD symptoms can appear in the mouth, on the tongue, along the gums, or in the throat — and they often look a lot like common, everyday conditions. A sore throat, a mouth ulcer, or a small bump inside the cheek can each have many causes, which makes it genuinely difficult to know when an oral STD might be involved. This page breaks down the symptoms associated with oral STDs by infection type, explains how soon those symptoms tend to appear, and walks through how testing works. For a broader look at what STDs can cause across the body, the complete guide to STD symptoms covers the full picture.
How STDs Start in the Mouth
An oral STD develops when a sexually transmitted infection reaches the mouth or throat through sexual contact. This typically happens during oral sex — either giving or receiving. When a partner has a genital or rectal infection, the same bacteria or virus can establish itself in the oral cavity.
The reverse is also possible. If someone has an oral herpes or gonorrhea infection, for example, that infection can be passed to a partner’s genitals through oral contact. Some infections can exist in more than one location at the same time — the throat and the genitals simultaneously, for instance.
The mouth and throat have mucous membranes that are vulnerable to the same pathogens that affect genital tissue. Bacteria like gonorrhea and chlamydia can colonize the throat. Viruses like herpes simplex can take hold on the lips, tongue, or inside the cheeks. The biology is similar — the location just happens to be different.
What Oral STD Symptoms Actually Look Like
The visible signs of an oral STD vary depending on the specific infection. Some produce very noticeable symptoms. Others produce nothing at all. Knowing what each type of symptom looks like — and which infections tend to cause them — makes the picture clearer.
Sores, Ulcers, and Blisters
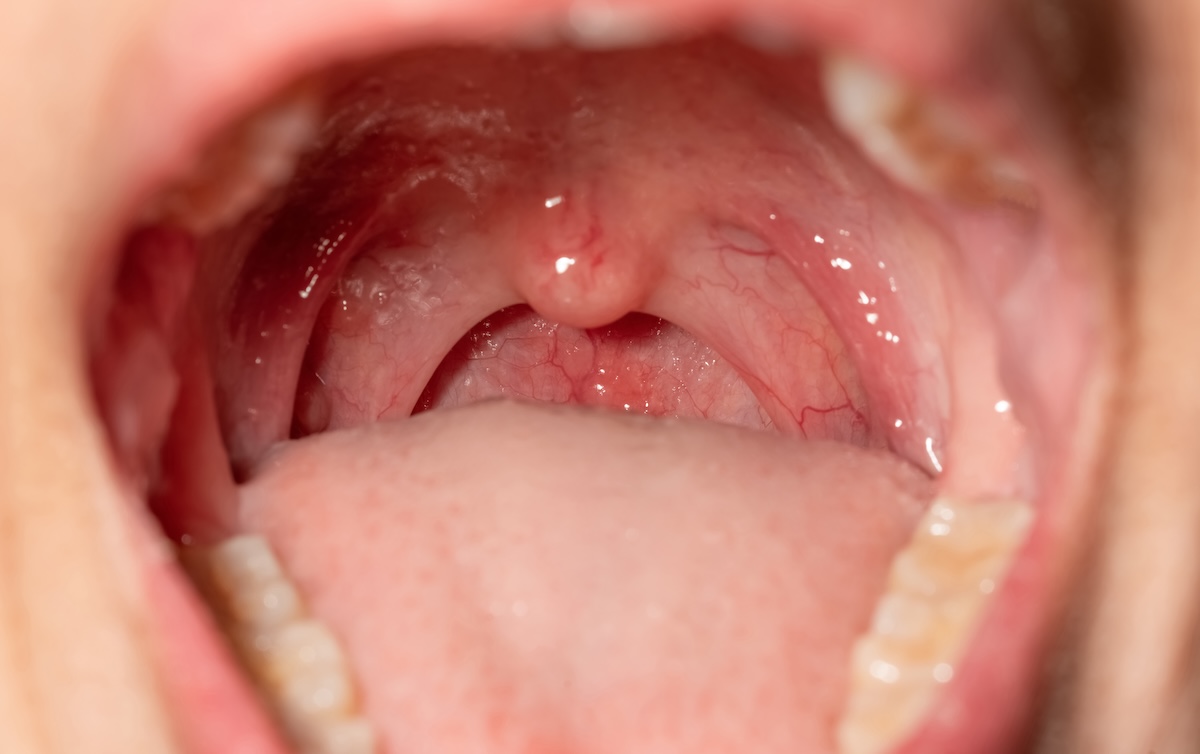
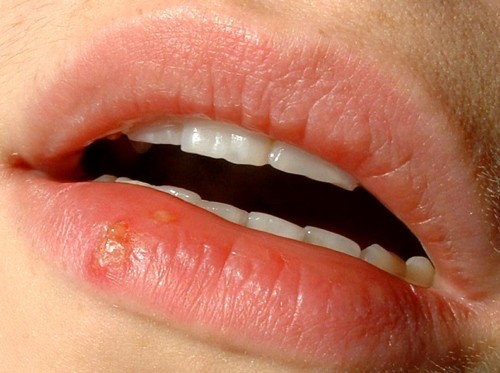
Open sores or ulcers in the mouth are one of the more distinctive oral STD symptoms. They can appear on the lips, tongue, gums, the inside of the cheeks, or the roof of the mouth. Depending on the infection, these sores may be painful or completely painless.
Herpes sores tend to be painful and often start with a tingling or burning sensation before blisters form. Syphilis sores — called chancres — are typically painless and round with a firm edge. Both types are contagious regardless of whether they cause discomfort.
White or Red Patches
White patches in the mouth can signal oral thrush, a fungal overgrowth that sometimes develops in people with immune system changes, including those living with HIV. These patches may appear on the tongue, the inner cheeks, or the roof of the mouth. Red patches in the same locations can also indicate infection.
Not every white patch in the mouth is an STD-related symptom — many have unrelated causes. But when white patches appear alongside other symptoms or after a potential exposure, testing provides the clearest answer.
Warts or Small Bumps
HPV can produce small, soft warts inside the mouth or throat. These are typically skin-colored or slightly gray, and they may appear in clusters. They’re often painless and easy to overlook.
Sore Throat That Doesn’t Resolve
A persistent sore throat that lingers without an obvious cause — such as a cold or flu — can sometimes be connected to an oral STD. Gonorrhea and chlamydia in the throat often present this way. A sore throat caused by STDs is more common than many people expect and is frequently mistaken for an ordinary illness.
Swollen Lymph Nodes
Swollen glands in the neck or under the jaw are a general sign that the immune system is responding to something. They can accompany several oral STDs, including herpes during an initial outbreak and syphilis during its early stages. Swollen lymph nodes alone aren’t specific enough to identify any particular infection — they’re a signal worth paying attention to alongside other symptoms.
Difficulty Swallowing
When throat inflammation is significant, swallowing can become uncomfortable. This symptom tends to occur with gonorrhea or chlamydia in the throat, particularly if the infection has been present for some time without being identified.
Oral STD Symptoms by Infection Type
Different infections produce different patterns of symptoms. The table below summarizes what each common oral STD tends to look like, along with typical timing for when symptoms might appear.
| Infection | Common Oral Symptoms | Often Asymptomatic? | Typical Symptom Window |
|---|---|---|---|
| Gonorrhea | Sore throat, burning sensation, swollen glands, occasional white spots | Yes — often | 1–14 days after exposure |
| Chlamydia | Sore throat, mild fever, swollen glands — often no symptoms at all | Yes — very commonly | 7–21 days after exposure |
| Herpes (HSV-1 / HSV-2) | Tingling, burning, blisters on lips or inside mouth, cold sores | Sometimes | 2–12 days after exposure |
| Syphilis | Painless sore (chancre) on lips or inside mouth, rash later | Sometimes | 10–90 days after exposure; average ~21 days |
| HPV | Small warts in mouth or throat, often no symptoms | Yes — frequently | Weeks to months; often much longer |
| HIV | Oral thrush (white patches), mouth ulcers — typically later presentations | Early infection may be silent | Oral signs often appear later in infection |
How Soon Do Oral STD Symptoms Appear?
The time between exposure and any symptoms showing up — called the incubation period — varies by infection. Some oral STDs can produce symptoms within a few days. Others take weeks. And some never produce noticeable symptoms at all, regardless of how long the infection has been present.
Gonorrhea in the throat can produce symptoms in as little as one day or up to about two weeks after exposure. Herpes typically produces its first outbreak somewhere between two and twelve days after initial exposure. Syphilis can take anywhere from ten to ninety days before a sore appears — the average is around three weeks.
Chlamydia in the throat tends to take one to three weeks before any symptoms appear, if they appear at all. HPV has a particularly long and variable window — warts may not develop for weeks, months, or sometimes much longer after exposure.
This variability is one of the main reasons symptoms alone aren’t a reliable indicator of whether an infection is present. Testing is the only way to confirm what’s actually going on.
What Oral Gonorrhea Looks Like
Oral gonorrhea is one of the more common oral STDs, and it’s also one of the hardest to detect by symptoms alone. The infection settles in the throat after sexual contact and can remain there without producing anything noticeable.
When symptoms do appear, the most common sign is a sore or burning sensation in the throat — similar to the feeling of a mild strep infection. Swollen lymph nodes in the neck may also develop. Occasionally, white spots appear in the mouth or on the tonsils. For a detailed breakdown of how this infection works and how it’s tested, oral gonorrhea explained covers the specifics.
Because throat gonorrhea so often produces either no symptoms or very mild ones, many people don’t realize they have it. A throat swab is the standard way to test for it — standard urine or blood panels won’t detect a throat infection.
What Are the First Signs of Oral Chlamydia?
Oral chlamydia is less commonly discussed than genital chlamydia, but it can develop after oral sexual contact with an infected partner. When it does produce symptoms, those symptoms tend to be mild and easy to dismiss.
The first signs of oral chlamydia — when they appear at all — include a mild sore throat, low-grade fever, and swollen glands in the neck. These symptoms overlap significantly with a common cold or mild throat infection, which is part of why oral chlamydia frequently goes undetected without testing.
Many people with oral chlamydia have no symptoms at all. For a more detailed look at what this infection looks like and how it’s diagnosed, chlamydia in the mouth provides a fuller explanation. Diagnosis is made through a throat swab, not through a standard urine test.
Can You Tell If You Have an Oral STD Without Testing?
Honestly, it’s very difficult. The most common oral STD symptoms — sore throat, mild mouth irritation, occasional swelling — overlap heavily with everyday infections and non-STD conditions. And a significant number of oral STDs produce no symptoms at all.
Herpes is perhaps the most visually recognizable oral STD because of its distinctive blistering pattern. Syphilis chancres in the mouth are also relatively distinctive. But both can be mistaken for other types of sores, and both can be present without producing visible signs.
The only reliable way to know whether an oral STD is present is through testing. Testing takes the guesswork out of it entirely and gives you a clear, confirmed answer.
How Oral STD Testing Works
Testing for oral STDs typically involves a throat swab rather than a blood draw or urine sample. The swab collects cells or fluid from the back of the throat, which are then tested in a lab for specific pathogens.
Different infections require different tests. A throat swab can detect gonorrhea and chlamydia in the throat. Herpes may be diagnosed through a swab of an active sore — if no sore is present, a blood test can detect herpes antibodies. Syphilis is tested through a blood draw. HIV is also detected through a blood test or, in some cases, an oral fluid test.
It’s worth noting that standard STD panels don’t automatically include throat testing. If you’ve had oral sexual contact and are concerned about a throat infection specifically, it’s a good idea to mention that when choosing a test — so the right sample type gets collected. You can find confidential STD testing near you to get the appropriate screening.
When Are Tests Accurate?
Test accuracy depends on the infection and on timing. Testing too soon after an exposure — before the infection has had time to establish itself — can produce a false negative result even when an infection is actually present. This window between exposure and when a test becomes reliable is called the window period.
For gonorrhea and chlamydia in the throat, tests are generally accurate within one to two weeks of exposure. For herpes, a blood antibody test becomes reliable around 12–16 weeks after a potential exposure. For syphilis, the window is around three to six weeks. For HIV, most tests are reliable by 45 days, with conclusive results typically available by 90 days.
If you test early and get a negative result, a follow-up test after the window period closes gives a more definitive answer.
Many Oral STDs Have No Symptoms at All
This point is worth expanding on because it often surprises people. Studies consistently show that oral gonorrhea is asymptomatic in the majority of cases. Oral chlamydia frequently produces no noticeable symptoms. Even herpes can be present without causing visible outbreaks — a state called asymptomatic shedding.
The absence of symptoms doesn’t mean the absence of infection. It simply means the body isn’t producing outward signs. An infection can still be present and detectable through testing even when nothing seems out of the ordinary.
This is one of the main reasons testing after a potential exposure makes sense regardless of whether symptoms are present. Symptoms are an unreliable guide to what’s actually happening.
How Common Are STDs from Oral Sex?
Oral sex does carry a lower overall transmission probability for many STDs compared to anal or vaginal sex. But “lower” doesn’t mean negligible, and certain infections — particularly gonorrhea — transmit fairly readily through oral contact.
Gonorrhea is among the most commonly transmitted STDs through oral sex. Studies have found that throat gonorrhea can be acquired from a single exposure. Herpes transmits through oral contact as well, particularly when an active sore is present — though transmission can also happen without visible symptoms. Syphilis, chlamydia, and HPV can also pass through oral sex.
The specific probability varies by infection, by role in the encounter (giving versus receiving oral sex), and by whether any cuts, sores, or inflammation are present in the mouth. No general number applies cleanly across all infections.
Do Oral STD Symptoms Differ Between Men and Women?
When it comes to oral and throat symptoms specifically, the differences are minimal. The same bacteria and viruses behave similarly in the oral cavity regardless of biological sex. A sore throat caused by gonorrhea looks the same whether it develops in a man or a woman. Herpes blisters on the lips follow the same pattern.
Where differences do emerge is in the broader context of an infection — genital symptoms, for example, can differ between sexes. But the oral presentation of the same infection tends to be consistent across sexes. The timing of symptoms and the likelihood of being asymptomatic are also comparable.
Can Oral STDs Clear Up on Their Own?
This depends significantly on the type of infection. Bacterial STDs — including gonorrhea, chlamydia, and syphilis — are caused by bacteria that don’t typically resolve without treatment. Waiting for them to go away on their own is generally not effective, and the infection remains detectable and transmissible in the meantime.
Viral infections work differently. Herpes is a lifelong virus that stays in the body — symptoms may come and go, but the virus itself doesn’t clear. HPV is an interesting case: the immune system does clear many HPV infections over time, often within one to two years, though certain strains persist longer.
Symptoms — if they appear at all — may fade temporarily with any of these infections, which can create the impression that the infection has resolved. But fading symptoms aren’t the same as a cleared infection. Testing is the only way to confirm status.
What to Do If You Notice Oral Symptoms
If you’ve noticed something that might be an oral STD symptom — an unusual sore, a persistent sore throat, a bump on your tongue, or white patches in your mouth — the most grounded next step is simply to find out what it is. Trying to diagnose it visually or by symptoms alone often leads to more uncertainty, not less.
Testing removes that uncertainty. A throat swab for gonorrhea and chlamydia, a blood test for syphilis and HIV, and a swab of any active sore for herpes together cover the most common oral STD possibilities. Many testing centers offer panels that combine multiple tests so you don’t have to choose each one individually.
Timing matters — testing right after an exposure may not yet be accurate, depending on the infection. If you’ve had a recent potential exposure, a testing center can help clarify which tests make sense and when to take them.
Not sure when to test? When you’re ready, find confidential STD testing clinics near you – same day appointments, no referral needed, results in 3 business days.
Frequently Asked Questions
How can I tell if I have an oral STD?
Oral STD symptoms — when they appear — can include a persistent sore throat, sores or blisters in the mouth, swollen lymph nodes in the neck, white patches on the tongue, or small warts inside the mouth or throat. The challenge is that many of these signs overlap with non-STD conditions, and many oral STDs produce no symptoms at all. Testing with a throat swab or appropriate blood test is the clearest way to find out.
How soon do oral STD symptoms appear after exposure?
The timing varies by infection. Gonorrhea symptoms can appear in as few as one to fourteen days. Herpes tends to show its first signs within two to twelve days. Syphilis typically takes between ten and ninety days, averaging around three weeks. Chlamydia symptoms, if they develop, usually appear within one to three weeks. Some infections, particularly HPV, may not produce any visible signs for months or longer.
What does oral gonorrhea look like?
Oral gonorrhea most commonly causes a soreness or burning sensation in the throat. Swollen glands in the neck may develop, and occasionally white spots appear in the mouth or on the tonsils. In many cases, oral gonorrhea produces no visible symptoms at all, making it difficult to detect without a throat swab test.
What are the first signs of oral chlamydia?
When oral chlamydia does produce symptoms, they tend to include a mild sore throat, low-grade fever, and slightly swollen glands. These signs are subtle and easily mistaken for a minor throat infection. A large proportion of oral chlamydia cases are completely asymptomatic, which is why testing is the most reliable way to confirm whether the infection is present.
Can oral STDs clear up without treatment?
Bacterial oral STDs — gonorrhea, chlamydia, and syphilis — generally don’t resolve on their own. They remain present and detectable without treatment. Viral infections like herpes stay in the body long-term, though symptoms may subside between outbreaks. HPV clears naturally in many cases over one to two years, but this isn’t guaranteed. Symptoms fading doesn’t confirm that an infection is gone.
Does oral STD testing require a throat swab?
Yes, for bacterial infections like gonorrhea and chlamydia in the throat, a throat swab is required. Standard urine or blood panels won’t detect a throat-based infection. Herpes can be swabbed from an active sore or tested through a blood antibody test. Syphilis and HIV are typically detected through blood tests. When you’re concerned about oral exposure specifically, it’s helpful to confirm with the testing center that throat sampling is part of the panel.
Is a sore throat always a sign of an oral STD?
No. A sore throat has many possible causes, including the common cold, strep throat, allergies, and acid reflux. An STD-related sore throat isn’t inherently distinguishable from other causes by feel alone. If a sore throat persists without a clear explanation and you’ve had recent oral sexual contact, a throat swab can rule an STD in or out. For more detail on this topic, STDs and sore throat explains the connection further.
Do oral STD symptoms look different in men versus women?
In the oral cavity and throat specifically, the presentation is generally consistent across sexes. The same bacteria and viruses behave similarly in the mouth regardless of biological sex. Differences in STD presentation between men and women tend to appear in genital symptoms, not in oral or throat symptoms.
Confidential, Private and Affordable STD Testing
Not sure when to test? Understanding your STD testing window period helps you get accurate results. When you're ready, find confidential STD testing clinics near you — same day appointments, no referral needed, results in 3 business days.