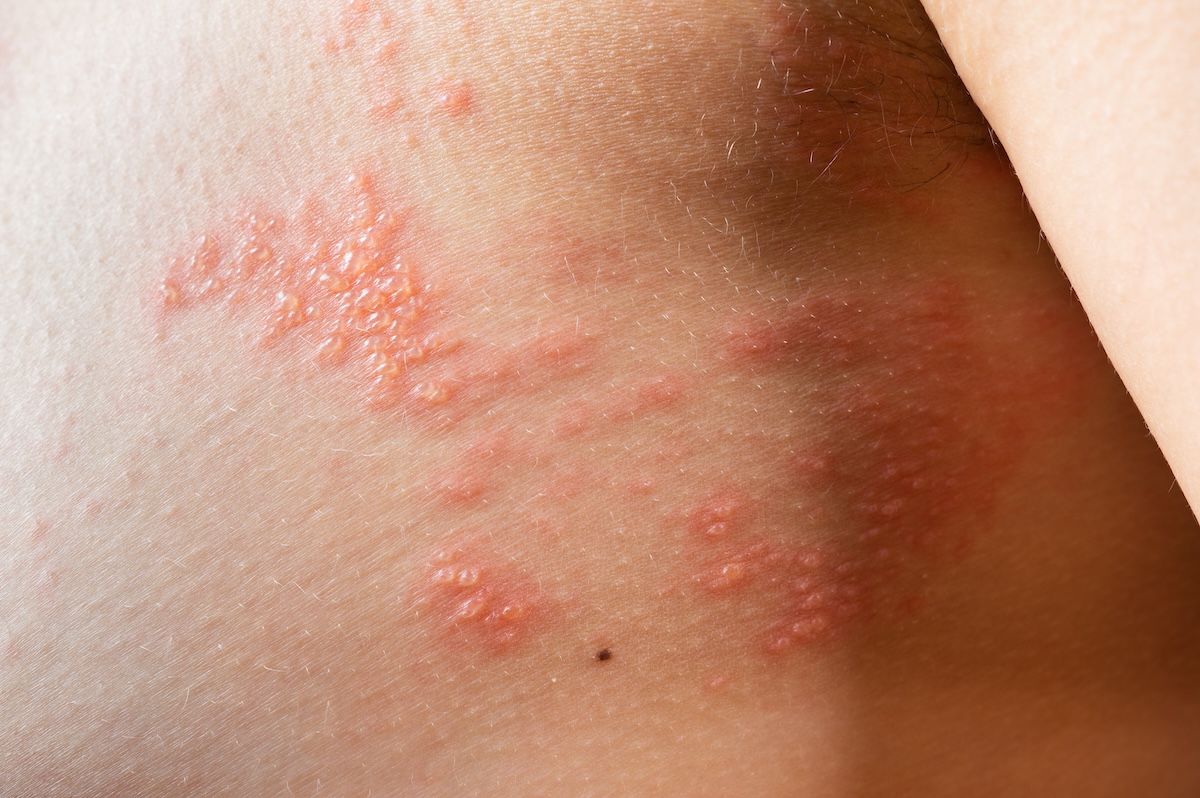
The herpes transmission rate is something a lot of people want to understand clearly — not as a source of worry, but as a way to make sense of their situation. Whether you’ve had a potential exposure, you’re in a relationship with someone who has herpes, or you’re just curious about the numbers, the actual data is more nuanced than most people expect. This page breaks down transmission rates by type, direction, and activity using peer-reviewed research.
For broader context on how STDs spread in general, the complete guide to STD transmission covers the full picture across multiple infections.
What the Numbers Actually Show
Herpes transmission rates vary quite a bit depending on the type of herpes, the direction of transmission, and what protective measures are in place. The overall annual risk for genital HSV-2 transmission between partners — where one partner has it and the other doesn’t — sits at roughly 10% per year without any protective measures.
That’s about a 1-in-10 chance over the course of a full year of regular sexual activity. Per individual sexual encounter, the numbers are considerably lower. A widely cited study published in the Journal of the American Medical Association found the per-act transmission risk for genital HSV-2 was approximately 0.04% female to male and 0.08% male to female per unprotected sex act.
Put another way, the odds of transmission from a single encounter with an infected partner are quite low — though they do add up over time.
HSV-1 vs. HSV-2 Transmission Rates
HSV-1 and HSV-2 behave differently when it comes to transmission, and the location of the infection matters.
What is the transmission risk of HSV-1?
HSV-1 is most commonly associated with oral herpes — cold sores around the mouth. It transmits readily through kissing and oral contact. Estimates suggest that around 67% of the global population under 50 carries HSV-1, though the majority never experience noticeable symptoms.
When HSV-1 is transmitted to the genitals through oral sex, the transmission rate exists but tends to be lower than genital HSV-2. Genital HSV-1 also sheds less frequently than genital HSV-2, which affects how often it passes between partners over time.
Can I still kiss someone with HSV-1?
Kissing someone with oral HSV-1 does carry a chance of transmission, particularly during or around an active cold sore. Outside of active outbreaks, viral shedding still occurs, though less frequently. The chance of transmission from a single kiss is low, but over many years of close contact, transmission is common — which is why HSV-1 prevalence is so high globally.
HSV-2 transmission rates by gender
Research consistently shows that male-to-female transmission of genital HSV-2 happens more easily than female-to-male transmission. Studies estimate the annual risk from an infected male to an uninfected female at around 16–17%, compared to roughly 4–8% from an infected female to an uninfected male.
This directional difference comes down to anatomy and the larger mucosal surface area exposed during sex.
Transmission Rates by Activity and Scenario
Understanding how herpes is transmitted by specific activity helps put individual situations in clearer perspective.
| Scenario | Estimated Transmission Risk | Notes |
|---|---|---|
| Annual risk (HSV-2, no protection) | ~10% per year | Between discordant couples |
| Male to female, per sex act (unprotected) | ~0.08% per act | Genital HSV-2 |
| Female to male, per sex act (unprotected) | ~0.04% per act | Genital HSV-2 |
| With daily antiviral medication | ~50% reduction overall | Valacyclovir studied in clinical trials |
| With consistent condom use (female partners) | Up to 96% reduction | From infected male to female |
| With consistent condom use (male partners) | ~65% reduction | From infected female to male |
| Condoms + daily antivirals combined | ~1–2.5% annual risk | Lowest documented rates in discordant couples |
| Oral sex (HSV-1 to genitals) | Lower than genital HSV-2 | Exact per-act data limited |
| Female to female transmission | Lower overall, data limited | Transmission through genital-to-genital contact possible |
What are the odds of getting herpes from a one-night encounter?
For a single unprotected sexual encounter with a partner who has genital HSV-2, the per-act risk is estimated at roughly 0.04% to 0.08% depending on the direction of transmission. That’s a very low absolute risk per individual exposure.
If a partner is on daily antiviral medication, those odds drop further. If condoms are also used, the risk reduces substantially again. No combination eliminates the possibility entirely, but the numbers show that a single encounter carries a much lower probability than many people assume.
When Is Herpes Most Contagious?
Herpes is most likely to transmit during an active outbreak, when the virus is present on the skin at its highest concentrations. Direct skin-to-skin contact with an active sore carries the highest per-contact transmission probability.
Outside of outbreaks, transmission still happens through asymptomatic viral shedding — when the virus is present on the skin surface without any visible signs. Research suggests approximately 70% of herpes transmissions occur during these asymptomatic periods, simply because most sexual activity happens when neither partner sees any visible sores.
HSV-2 sheds asymptomatically more often than HSV-1 in the genital region, which is one reason genital HSV-2 transmits more frequently over time than genital HSV-1.
How Medication and Condoms Affect the Rates
The data on risk reduction is genuinely encouraging. Daily antiviral medication — most commonly Valacyclovir — reduces the rate of viral shedding, which in turn lowers the chance of transmission to a partner by approximately 50%.
Consistent condom use adds another layer. Studies show condoms reduce the risk of transmission to female partners by up to 96%, and to male partners by around 65%. The difference in effectiveness comes down to how much skin is covered relative to where the virus sheds.
When both measures are combined — daily antivirals and consistent condom use — the annual transmission risk in discordant couples drops to somewhere in the range of 1–2.5%. That’s a substantial reduction from the baseline 10% annual figure.
Is there medicine to prevent getting herpes?
There’s currently no approved medication that prevents herpes infection in someone who doesn’t have it — in the way that PrEP works for HIV. What antiviral medications do is suppress viral activity in someone who already has herpes, which lowers the likelihood they’ll pass it to a partner. Valacyclovir is the most widely studied option for this purpose, and it works by reducing both the frequency of outbreaks and the rate of asymptomatic shedding.
Is It True That 90% of People Have Herpes?
The figure that gets cited varies depending on which type is being counted and which age group is measured. For HSV-1, global prevalence among adults under 50 is estimated at around 67% by the World Health Organization. When older age groups are included, the number rises. For HSV-2, global prevalence is estimated at around 11% of the population aged 15–49.
The “90%” figure tends to be an overstatement, but it reflects the fact that HSV-1 in particular is genuinely very common — often acquired in childhood through non-sexual contact. Many people carry the virus and have never had a noticeable symptom.
Will Herpes Ever Be Cured?
As of now, there’s no cure for herpes. Once the virus establishes itself in nerve cells, it stays in the body. Antiviral medications manage the virus effectively — reducing outbreaks, lowering shedding rates, and decreasing transmission probability — but they don’t eliminate the infection.
Research into herpes vaccines and gene-editing approaches is ongoing, and there has been meaningful progress in recent years. But no cure is currently available or approved.
Testing After a Potential Exposure
If you’ve had a potential exposure and want clarity, herpes 1 and 2 blood testing can identify whether HSV-1 or HSV-2 antibodies are present. Blood tests look for IgG antibodies, which the body produces in response to the virus.
Timing matters with herpes testing. After a first exposure, it can take 12–16 weeks for antibodies to reach detectable levels. Testing too early may return a negative result even if infection is present. A test taken at least 12 weeks post-exposure gives a more accurate picture, and retesting at 16 weeks provides the most reliable result.
Swab testing of an active sore can confirm an infection faster — usually within days of an outbreak appearing — since it detects viral DNA directly rather than waiting for an antibody response.
Find a testing location near you
Frequently Asked Questions
What is the annual herpes transmission rate for couples?
For couples where one partner has genital HSV-2 and the other doesn’t, the estimated annual transmission rate is around 10% without any protective measures. That figure drops significantly — to roughly 1–2.5% — when both daily antiviral medication and consistent condom use are combined.
What is the HSV-2 transmission probability female to male?
Research estimates female-to-male genital HSV-2 transmission at approximately 0.04% per unprotected sex act, or around 4–8% annually. This is lower than the male-to-female rate, which is generally attributed to anatomical differences in mucosal exposure.
What are the chances of getting herpes from one encounter?
The per-act transmission risk for genital HSV-2 is estimated at roughly 0.04% to 0.08% depending on the direction. For a single encounter, the absolute probability is low — though it’s higher if the partner is experiencing an active outbreak at the time.
How much does Valacyclovir reduce herpes transmission?
Clinical trials have shown that daily Valacyclovir reduces the risk of transmitting genital HSV-2 to a partner by approximately 50%. It works by reducing both the frequency of outbreaks and the rate of asymptomatic viral shedding between outbreaks.
When should I test after a herpes exposure?
Blood tests for herpes detect IgG antibodies, which take time to develop. Testing at 12 weeks post-exposure gives a reasonably accurate result, while 16 weeks is considered the most reliable window. If an active sore is present, a swab test can give a result much sooner.
Can herpes transmit without symptoms?
Yes. Approximately 70% of herpes transmissions are estimated to occur when the infected partner has no visible symptoms — a process called asymptomatic viral shedding. This is one reason herpes continues to spread even among people who don’t know they have it.
Is female-to-female herpes transmission possible?
Yes, female-to-female transmission of herpes is possible through genital-to-genital skin contact. The exact transmission rate is less well-studied than heterosexual transmission data, but the same underlying mechanism — direct contact with an area where the virus is active — applies.
Does a single positive herpes test always mean recent transmission?
Not necessarily. A positive IgG blood test shows that antibodies are present, but it doesn’t pinpoint when infection occurred. Many people test positive and have carried the virus for years without realizing it. If timing is a concern, discussing the result with a healthcare provider can help clarify what the test result means in context.
Understanding the actual numbers around herpes transmission tends to make the topic feel a lot less overwhelming. The data shows that per-encounter risks are genuinely low, and that risk reduction measures can bring those numbers down further. Whatever your situation, getting clear information is always a reasonable place to start.
Confidential, Private and Affordable STD Testing
Not sure when to test? Understanding your STD testing window period helps you get accurate results. When you're ready, find confidential STD testing clinics near you — same day appointments, no referral needed, results in 3 business days.